😣Navigating the Emotional Rollercoaster: Understanding Borderline Personality Disorder (BPD)
Understanding Borderline Personality Disorder: Symptoms, Causes, and Treatment
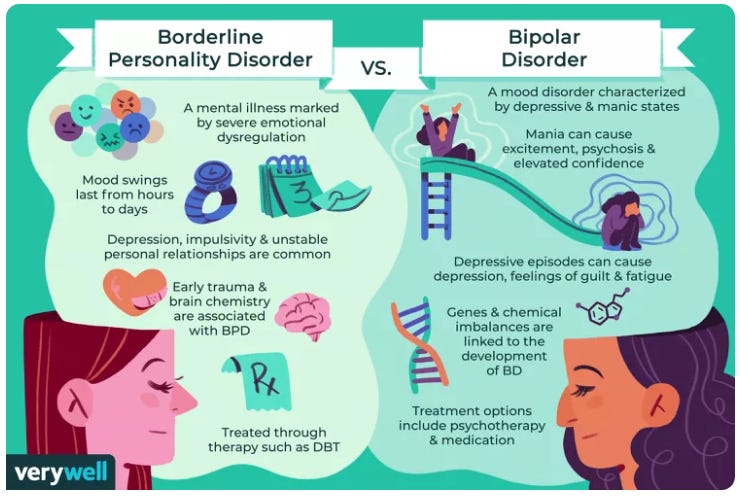
Are you aware of other conditions that share similarities with BPD and can often be mistaken for it?
Find out the differences here.
Meet Alex (Bipolar Disorder) John, a 35-year-old man, experiences distinct periods of elevated mood, known as manic episodes, followed by episodes of depression. During his manic episodes, he exhibits increased energy, racing thoughts, and engages in impulsive activities, such as excessive spending or risky behavior. However, unlike individuals with BPD, Alex’s mood swings are typically more prolonged and distinct, lasting for days or weeks. Additionally, his mood shifts are not triggered by fear of abandonment or a distorted self-image, which are characteristic of BPD.
Sarah (Borderline Personality Disorder - BPD) Sarah, a 30-year-old woman, struggles with intense mood swings, unstable relationships, and chronic feelings of emptiness. She frequently engages in impulsive behaviors, such as reckless spending and self-harm. Sarah has a distorted self-image and often experiences fears of abandonment. Her emotions can rapidly shift from extreme anger to deep sadness within a short period. It is crucial to note that while Sarah may exhibit some symptoms that overlap with other disorders, her persistent pattern of emotional instability, self-destructive behaviors, and intense fear of abandonment aligns more closely with Borderline Personality Disorder (BPD).
Then, Lisa (Dependent Personality Disorder) Lisa, a 28-year-old woman, constantly seeks reassurance and approval from others. She has an overwhelming fear of being alone and relies heavily on others to make decisions for her. Lisa's self-esteem is highly dependent on others' opinions, and she struggles to take initiative or make independent choices. While Lisa may exhibit some emotional instability, her primary symptoms revolve around an excessive need for support and guidance from others, distinguishing her case from Borderline Personality Disorder.
This is Emily (Post-Traumatic Stress Disorder - PTSD) Emily, a 32-year-old woman, experiences intrusive thoughts, nightmares, and flashbacks related to a traumatic event she endured in the past. These symptoms are triggered by specific cues or reminders associated with the trauma. Emily may exhibit emotional dysregulation and occasional impulsive behavior as a result of her trauma, but her symptoms are predominantly related to re-experiencing the traumatic event, rather than the chronic patterns of emotional instability and relationship difficulties seen in BPD.
It's important to note that these are simplified examples, and a comprehensive assessment by a qualified mental health professional is necessary to provide an accurate diagnosis and develop an appropriate treatment plan. Each disorder has distinct diagnostic criteria and treatment approaches, highlighting the significance of a thorough evaluation.
History of BPD
Borderline Personality Disorder (BPD) has a complex and evolving history within the field of mental health. The term "borderline" was first used in the early 20th century to describe patients who fell on the "borderline" between neurosis and psychosis. In the 1930s, the concept of "borderline schizophrenia" emerged, but it was later recognized as a distinct condition.
In the 1960s, the diagnosis of Borderline Personality Organization was introduced by psychoanalyst Otto Kernberg, who highlighted the disorder's core features of identity diffusion, splitting, and primitive defense mechanisms. However, it wasn't until the 1980s that BPD was officially recognized as a distinct diagnostic category in the Diagnostic and Statistical Manual of Mental Disorders (DSM-III).
Since its inclusion in the DSM, there have been ongoing debates and refinements in defining the diagnostic criteria for BPD. The understanding of BPD has shifted from a primarily psychoanalytic perspective to a more comprehensive and multidimensional view. This evolution has resulted in a broader recognition of the biological, genetic, environmental, and interpersonal factors that contribute to the development and maintenance of BPD.
Over the years, advancements in research and clinical practice have led to improved diagnostic accuracy and more effective treatment options for individuals with BPD. Psychotherapy, particularly Dialectical Behavior Therapy (DBT), has shown promising results in helping individuals with BPD manage their emotions, improve relationships, and enhance their overall quality of life.
As our understanding of BPD continues to grow, efforts are being made to reduce the stigma associated with the disorder and increase awareness and empathy for those who are affected. Ongoing research aims to uncover the underlying mechanisms of BPD and develop targeted interventions to support individuals living with this challenging condition.
What is Borderline Personality Disorder?
Borderline Personality Disorder (BPD) is a mental health condition characterized by a persistent pattern of unstable relationships, self-image, and emotions. People with BPD often struggle with intense mood swings, impulsivity, and a distorted sense of self. They may experience difficulty regulating their emotions, leading to relationship conflicts and a sense of chronic emptiness.
Symptoms
Emotional instability: Individuals with BPD may experience intense and rapidly shifting emotions, such as anger, anxiety, or sadness. These emotional fluctuations can occur in response to minor triggers and are often challenging to control.
Unstable relationships: People with BPD may have difficulties maintaining stable and healthy relationships due to their fear of abandonment, idealization followed by devaluation, and a tendency to push others away.
Impulsivity: BPD is often associated with impulsive behaviors such as reckless spending, substance abuse, binge eating, self-harm, or unsafe sex.
Distorted self-image: Individuals with BPD may struggle with a persistent and unstable sense of self. They may have an unclear understanding of their goals, values, and preferences.
Chronic feelings of emptiness: Many individuals with BPD describe a deep sense of inner emptiness and a longing for something they cannot quite define.
Self-destructive behaviors: BPD is linked to self-harming behaviors, suicidal thoughts, or suicide attempts. These behaviors often serve as a desperate attempt to cope with overwhelming emotions.
Causes
The exact cause of BPD is still not fully understood, but research suggests a combination of genetic, environmental, and neurological factors. Traumatic experiences, such as childhood abuse or neglect, can significantly contribute to the development of BPD. Additionally, certain brain abnormalities and imbalances in neurotransmitters may play a role in the manifestation of the disorder.
Herbal Treatment
While there is no specific herbal treatment that can cure BPD, some complementary approaches may aid in managing symptoms. It is crucial to note that herbal remedies should never replace professional mental health care, but they can be used as complementary support. Herbs such as chamomile, lavender, and valerian root are known for their calming properties and may help reduce anxiety and promote relaxation. However, it is essential to consult with a qualified healthcare practitioner before incorporating any herbal remedies into a treatment plan.
Diseases Related to BPD
Major Depressive Disorder: Many individuals with BPD also experience depressive episodes, characterized by persistent sadness, loss of interest, and feelings of hopelessness.
Anxiety Disorders: BPD often coexists with anxiety disorders, such as generalized anxiety disorder, social anxiety disorder, or panic disorder.
Substance Use Disorders: Due to impulsivity and emotional dysregulation, individuals with BPD are at an increased risk of developing substance abuse problems.
Eating Disorders: BPD is frequently associated with eating disorders, such as binge eating disorder, bulimia nervosa, or anorexia nervosa.
"Though the road may be rocky, remember that every step forward is a victory. You have the strength to overcome the challenges of Borderline Personality Disorder and build a life filled with love and stability”
#BPDWarrior #MentalHealthMatters #BreakingTheStigma #FindingStability #HealingJourney